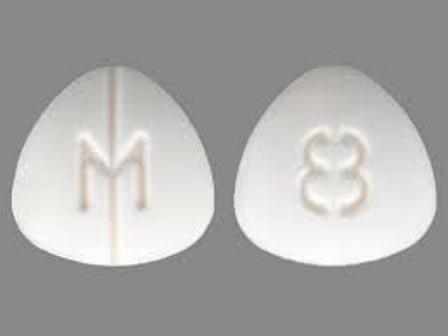
Dilaudid M8 8mg
£749.00
Dilaudid M8 8mg — Complete Guide, Uses, Effects, and Safety Considerations
Dilaudid M8 8mg is a potent opioid analgesic commonly prescribed for the treatment of moderate to severe pain. It contains hydromorphone, a semi-synthetic opioid that is significantly stronger than morphine. The 8mg dose, labeled as M8, is typically used for patients requiring substantial analgesic effects, such as those with severe post-surgical pain, cancer-related pain, or chronic pain that has not responded adequately to other opioids.
Due to its potency, Dilaudid M8 8mg carries a high risk of dependence, tolerance, and overdose, making it essential that the medication is used strictly under medical supervision. This comprehensive guide provides in-depth information on pharmacology, therapeutic uses, dosing, side effects, safety considerations, and public health concerns.

Historical Background
Hydromorphone, the active ingredient in Dilaudid, was first synthesized in the 1920s as a derivative of morphine, designed to provide a more potent analgesic with a potentially improved side effect profile. Over the decades, hydromorphone has become a mainstay in pain management, particularly in cases of severe pain where other opioids are insufficient.
-
1920s: Hydromorphone synthesized from morphine
-
1940s–1950s: Clinical introduction for severe pain management
-
1970s–2000s: Expanded use in cancer pain and palliative care
-
Present: Available in various formulations, including oral tablets, liquid solutions, and injections
Chemical and Pharmacological Profile
Chemical Structure
Hydromorphone is a semi-synthetic opioid with the chemical formula C17H19NO3. It is structurally related to morphine but has modifications that increase its potency and lipophilicity, allowing for faster penetration into the central nervous system (CNS).
Mechanism of Action
Hydromorphone exerts its effects primarily by agonizing mu-opioid receptors in the brain and spinal cord, which:
-
Reduces pain perception
-
Alters the emotional response to pain
-
Produces analgesia and mild euphoria
Its dual action on the CNS and spinal cord makes it particularly effective for severe pain management.
Potency and Onset
-
Oral onset: 15–30 minutes
-
Peak effect: 30–60 minutes
-
Duration: 3–6 hours for immediate-release formulations
-
M8 dose: Provides a strong analgesic effect suitable for opioid-tolerant patients or closely monitored opioid-naive patients
Medical Uses
Dilaudid M8 8mg is prescribed for:
-
Acute severe pain: Postoperative or trauma-related pain
-
Chronic pain: Severe musculoskeletal pain, cancer-related pain, neuropathic pain in selected cases
-
Breakthrough pain: Used as a supplement for patients already on long-acting opioids
It is especially valuable when other opioid medications, such as morphine or oxycodone, are insufficient or poorly tolerated.
Formulations
-
Immediate-release tablets
-
Oral liquid solutions
-
Injectable formulations (IV, subcutaneous, IM)
Dosage Guidelines
Adult Dosing
-
Immediate-release oral tablets: 2–8mg every 4–6 hours as needed for pain
-
Maximum daily dose: Determined by patient response and medical supervision
-
Titration: Adjusted to achieve effective analgesia while minimizing adverse effects
Special Considerations
-
Start with the lowest effective dose, particularly in opioid-naive patients
-
Monitor for respiratory depression, sedation, and other side effects
-
Adjust dose in patients with renal or hepatic impairment
Pharmacokinetics
Absorption
-
Rapid oral absorption
-
Peak plasma concentration within 30–60 minutes
Distribution
-
Widely distributed in body tissues, including the CNS
-
Crosses the placenta and is excreted in breast milk
-
Moderate protein binding (20–30%)
Metabolism
-
Primarily metabolized in the liver to hydromorphone-3-glucuronide
-
Minimal analgesic activity from metabolites, but accumulation may occur in renal impairment
Excretion
-
Excreted mainly through urine
-
Half-life: 2–3 hours for immediate-release tablets
-
Extended-release formulations last longer
Therapeutic Effects and Benefits
Dilaudid M8 8mg provides:
-
Rapid and effective relief from severe pain
-
Improved quality of life for patients with chronic or terminal illnesses
-
Sedative effects that reduce anxiety associated with pain
-
Versatile use in both inpatient and outpatient settings
Side Effects
Common Side Effects
-
Nausea and vomiting
-
Constipation
-
Drowsiness or sedation
-
Dizziness
-
Sweating
-
Dry mouth
Serious Side Effects
-
Respiratory depression (most critical risk)
-
Severe sedation
-
Hypotension or bradycardia
-
Confusion, delirium, or hallucinations
-
Allergic reactions
-
Seizures (rare)
Long-Term Concerns
-
Development of tolerance over time
-
Physical dependence
-
Opioid-induced hyperalgesia (increased sensitivity to pain)
Tolerance, Dependence, and Withdrawal
Tolerance
-
Over time, patients may require higher doses to achieve the same analgesic effect
-
Regular monitoring is essential
Dependence
-
Physical dependence can occur after continuous use for weeks or months
-
Abrupt cessation may trigger withdrawal symptoms
Withdrawal Symptoms
-
Anxiety, irritability, and restlessness
-
Insomnia and fatigue
-
Sweating and chills
-
Muscle aches
-
Nausea, vomiting, diarrhea
Tapering under medical supervision is recommended to minimize withdrawal risks.
Addiction Risk
-
High potential for misuse and addiction
-
Abuse may include crushing and snorting or injecting tablets
-
Signs of addiction include compulsive use despite harmful consequences
Overdose Risk and Safety Considerations
Signs of Overdose
-
Slow, shallow, or labored breathing
-
Extreme drowsiness or unresponsiveness
-
Pinpoint pupils
-
Low blood pressure
-
Cold, clammy skin
Risk Factors for Overdose
-
High or repeated doses
-
Concomitant use with alcohol or CNS depressants
-
Pre-existing respiratory or cardiovascular conditions
Treatment of Overdose
-
Immediate medical attention required
-
Naloxone can reverse opioid-induced respiratory depression
-
Supportive care includes oxygen, IV fluids, and monitoring vital signs
Safe Use Guidelines
-
Adhere strictly to prescription instructions
-
Avoid alcohol or sedating medications
-
Secure storage away from children
-
Do not share medication
-
Follow up regularly with a healthcare provider
Special Populations
-
Elderly patients: Increased sensitivity to sedation and respiratory depression; dose adjustments may be needed
-
Pregnant and breastfeeding women: Crosses placenta and breast milk; use only if benefits outweigh risks
-
Patients with respiratory disorders: Careful monitoring required
-
Renal or hepatic impairment: Dose reduction may be necessary
Drug Interactions
Dilaudid M8 8mg may interact with:
-
Other opioids
-
Benzodiazepines and sedatives
-
Alcohol
-
Certain antidepressants (may increase sedation or serotonin-related effects)
Medical supervision is crucial to prevent dangerous interactions.
Legal Status and Regulation
-
United States: Schedule II controlled substance
-
High potential for abuse
-
Strict prescribing regulations
-
-
Unauthorized possession, sale, or distribution is illegal and may carry severe penalties
-
Internationally, hydromorphone is tightly regulated due to abuse potential
Public Health Considerations
-
Misuse of hydromorphone contributes to the opioid crisis
-
Prescription monitoring programs help prevent diversion
-
Patient and caregiver education on safe use and storage is critical
-
Responsible prescribing balances effective pain relief with minimizing risk
Alternatives for Pain Management
-
Non-opioid analgesics: acetaminophen, NSAIDs
-
Adjuvant medications: gabapentin, pregabalin
-
Physical therapy and exercise
-
Cognitive-behavioral therapy for pain
-
Other opioids for opioid-tolerant patients: morphine, oxycodone, fentanyl
Conclusion
Dilaudid M8 8mg is a potent and effective analgesic for severe pain management. When used responsibly under medical supervision, it can significantly improve quality of life for patients with acute, chronic, or cancer-related pain.
Due to the high risk of tolerance, dependence, and overdose, careful monitoring, patient education, and adherence to dosing guidelines are essential. Proper use ensures maximum pain relief while minimizing risks associated with opioid therapy.
| Quantity | 100 |
|---|
Related products
Products
Products
Products
Products
Products
Products
Products
Products